“I’m not dead!” — Old peasant, Monty Python and the Holy Grail
Howdy, folks, I know we took last week off, but it is was mainly because I had to use my blog-research-time to road trip to my Covid vaccine appointment (finally— I live in Pennsylvania, where we’re just now thinking about leaving Phase 1a). But it did give me the idea to talk a little about ancient medicine, and what exactly that meant for the people of the Mediterranean. And, as usual, it behooves us to begin with Egypt.
Ancient Egyptian medicine is some of the oldest for which we have a continuous record. Egyptologists have recovered scores of medical papyri from tombs and the remains of Per-Ankhs, Houses of Life, which served as quasi-hospitals. Like all hieroglyphic texts, they remained indecipherable until the discovery of the Rosetta Stone in 1822, but once we had a grasp of the language, we’ve received a good idea of the breadth of Egyptian medical knowledge, which was largely unchanging until the Persian and Greek invasions of the middle of of the last century BC (500s-300s).

Unlike, say, medieval European medics, the one thing the ancient Egyptian doctors never lacked for was access to the human body. As you might surmise, the mummification process provided the Egyptians with ample opportunity to study organs and how they related to one another. They instinctively understood that the body systems flowed together much in the way their sacred Nile did, and blockages caused problems just as silted canals and droughts did. Because of this, Egyptian medical arts, like many ancient medicines, put a lot of focus on purgatives and laxatives, the better to remove perceived blockages. Proctologists were numerous and important enough that we even know their official title from the medical papyri: neru phuyt, literally, “the Shepherd of the Anus,” which is an almost kindly description of their practice.
Egyptian pharmacology was extensive, utilizing over 160 plants for a variety of ointments and potions. While modern analysis holds most of these mixtures as being largely ineffective, certain concoctions using common ingredients like castor oil, honey, and alcohol would have had therapeutic and antibacterial qualities. Egyptians also used cannabis much in the same way it is in increasingly used in modern medicine, and certain metals, which sounds unhelpful until you remember many vitamins and minerals are elemental metals. But unlike us, they also relied extensively on animal feces, which were probably less useful.
Mummification also reveals certain aspects of Egyptian medical knowledge through the choices made regarding which organs they chose preserve. Remember, Egyptians believed the body would be required intact in the afterlife, so if organs were believed to be needed, they, too, must be intact. The lungs, liver, stomach, and intestines were specially sealed in the so-called canopic jars and placed with a mummy in its tomb. Each jar was protected by its individual guardian, a son of the falcon god Horus (represented as the jar lid); a greater deity; and one of the cardinal directions. The lungs were protected by the baboon-faced Hapi, the funerary goddess Nephthys, and represented North. The liver belonged to the human-faced Imsety, Isis, and represented South. The stomach was protected by jackal-headed Duamutef, the mother goddess Neith, and represented East. Lastly, the intestines belonged to the falcon-headed Qebehsenuef, the West, and the scorpion goddess Selket (Serqet). Selket was already an important medical deity, given her place as the goddess who protected the Egyptians from both scorpions and snakes, as was Isis, who as the goddess of magic, which we’ve discussed was closely practiced alongside medicine.

While Egyptian physicians did not have the sophistication to discern the difference between veins, nerves, and muscles, they did have a rudimentary understanding of the cardiac system. They appear to have extrapolated that the blood transported nutrients and waste, even if they could not have named those elements as oxygen and carbon dioxide. They were also aware that pulse was connected to the heart (ib), and perceived the importance of that organ, which is why it was seen as the seat of a person’s being and intellect. The heart, which was believed to be required for the all-important weighing before Osiris, was seen as so important that unlike the canopic organs, it was embalmed and replaced within the body before it was wrapped, to prevent it being lost.

So, if the heart was the Egyptian seat of the intellect, where does that leave the brain? Well, rather famously, the Egyptians didn’t seem to understand the function of the brain, and would throw it away during the mummification process after extracting it from the skull through the nose. But if one takes their religious belief in the necessity of one’s organs for proper functioning in the afterlife at face value, the shuffling, zombie-like behavior of the classic monster mummy suddenly makes a lot of sense. How good will you get on if you’re brought back to life without your brain?

Ancient medicine of all stripes, with its ignorance of germ theory, generally avoided surgery whenever possible (one of the medical papyri warns off trying to excise tumors with the admonishment of “do thou nothing there against”), but that doesn’t mean surgery was unknown in Egyptian medicine. We’ve uncovered limb prostheses in tombs, and Egyptian medicine was deeply involved in dentistry in all of its forms. The desert put sand into everything, including food, and as a result, the Egyptians suffered from chronic, excessive wear on their teeth that was unknown among their northern and eastern neighbors. While improved grain grinding techniques would alleviate the severity of this the closer one moves toward to the Common Era, it would always be a part of Egyptian life. Egyptian dentists also dealt with other common oral problems such as extractions and cysts, although rarely cavities as the Egyptian diet was largely devoid of refined sugars.

There were many ranks of physicians in ancient Egypt, practicing a wide range of specialties. We already talked about Djoser’s court physician, Imhotep, whose great general knowledge made him a god upon his death, and those shepherding proctologists, but there were also gastroenterologists, gynecologists, and perhaps of interest to my God’s Wife readers, ophthalmologists. Ancient ocular prosthetics were fairly primitive, in case you were wondering why I chose a simple eyepatch for the character in question. In-socket eye prosthetics weren’t widespread until the sixteenth century, thanks to the Venetians and their expert glassworks, so ancient replacement eyes were largely made of gold or light clay and affixed over the socket with thin wire, perhaps of gold, much as an eyepatch would function.
Unlike many other parts of the ancient world, we also have evidence that there women doctors in Egypt. In the tomb of Akhethotep, a vizier of Fifth Dynasty pharaoh Djedkare (2400s BC), we have an inscription for his mother, Peseshet, describing her as a sewnewt. The Egyptian word for “doctor” is sewnew (swnw in the transliteration guidelines), the presence of the all-important t at the end of Peseshet’s title is a feminine suffix. This makes Dr. Peseshet the earliest woman doctor for whom we have a historical record— there is a famous woman physician, Merit-Ptah, who supposedly served the pharaonic court during the Second Dynasty (2700s BC), but she is now widely believed to be fictional. Of course, behind either of these women stand all of the midwives who have practiced their craft in every society since time immemorial, and have always struggled for the official recognition of their higher-ranking male colleagues.
If the ancient Egyptian approach to medicine interests you, I’d recommend Mika Waltari’s novel, The Egyptian, whose protagonist, Sinuhe, is a royal physician. Waltari did extensive research for this book, and his descriptions of Sinuhe’s training and work are generally considered accurate by experts.

By the time the Ptolemies ruled Egypt, thanks to Alexander the Great, most of the ancient Mediterranean had begun to use Greek medical thought as the basis of their diagnostics and treatment. The Greeks originally held beliefs ostensibly similar to the Egyptians, that illness was caused by divine disfavor or demonic interference, and the practices of the Asclepeia reflect this. The Asclepeia were temples dedicated to Asclepius, the Greek god of medicine and healing, the son of Apollo by a Greek princess named Coronis or Arsinoë, depending on which tradition you follow.

The Asclepeia served as convalescent houses, where physician-priests tended the sick through a variety of means, but especially enkoimesis (in Greek, ἐγκοίμησις), a sort of induced dream state, in which the patient might receive a message from the gods for the priests to interpret, or the hypnotic trance might simply allow them to operate on the patient with less trauma. This sounds much like modern hypnotherapy, but there is also evidence that the Asclepeia used less esoteric means of relief like opiates.

The big leap in Greek medical thought was the idea of humorism, espoused by the most famous of the ancient Greek physicians, Hippocrates (mid-400s – mid-300s BC). Hippocrates believed the body to be divided into four substances, or humors, that needed to be in balance for a person to be healthy. These were blood, phlegm, yellow bile, and black bile. Much like the canopic jars, each humor was linked to a particular organ, as well as a season, an element, and a personality type. Hence why if you’ve ever heard a person described as phlegmatic, that is, reserved and perhaps slow to action, that is connected to humorism. The Greeks would have said that person had an excess of the phlegm humor in their system that manifested in their personality. And indeed, there is some evidence that humorism, as much as we associate it with the Greeks, might have originally arisen out of Egyptian medical thought, or even out of traditional Ayurvedic medicine in ancient India, which divides the body in elemental spheres called doshas, and is still widely practiced in Southeast Asia as an alternative medicine alongside of modern Western-based medicine.

Under humorism, when the imbalance between the humors became too pronounced, a person would become sick and a physician would need to restore the balance of the humors to bring about recovery. This was generally achieved by blood letting, purges, enemas, and dietary changes. This viscous, elemental approach to medicine would be incredibly durable— adopted into Western and Islamic medical thought deep into the modern age. Indeed, it could be argued that humorism wasn’t truly defeated in Western medicine until the mid-19th century, and even then, it would still be employed by physicians trained on the classical Greek medical texts well into the struggling years of early germ theory in the early 20th century.
Greek physicians studying in Alexandria under the aegis of the Ptolemies would also make advances in the ancient world’s understanding of biology and anatomy. Herophilos of Chalcedon is considered one of the first medical teachers in Alexandria and one of the earliest western physicians to engage in systematic autopsies. Along with his contemporary, Erasistratus of Chios, he discerned the functions of the nervous system and brain, correctly placing control of the intellect and motor movements in their sphere. Herophilos also was able to differentiate veins and arteries, recognizing only the latter have a pulse, leading him to begin to understand their different functions in the circulatory system. Some of these discoveries were made from experimentation on animals, but as so often in medical history, Herophilos, Erasistratus, and their students were not above human experimentation. The Ptolemaic pharaohs often gave the medical schools condemned criminals, and much of their newfound knowledge of the body stemmed from observations made during painstaking vivisections of these prisoners.

Like so many things, the Romans generally adopted Greek medical practices, in part because many physicians in the late Republic and early Empire were themselves Greek. Despite Julius opening Roman citizenship to all physicians in 46 BC, medicine was not a particularly high-status profession, so foreigners and freedpeople were more likely to engage in it, although doctors who served the emperor’s household enjoyed a certain celebrity, like Musa in the entourage of Octavius, and later, Galen in the courts of Marcus Aurelius, Commodus, and Septimius Severus. Interestingly enough, medicine was also a profession open to women in Rome. Medicae and obstetrices, as the latter’s name implies, were more likely to serve as midwives and gynecologists than as general practitioners, but were seen as equally skilled as their male colleagues and were often literate at a time when not all women (or men) were.
Another Hippocratic idea adopted readily by the Romans was miasma theory, which postulated that epidemics were caused by noxious air or vapors that spread disease. We literally named malaria (mal–aria, “bad air”) after this concept. Ancient people understood that contaminated water and other unhygienic conditions led to plagues, as evidenced by Rome’s constant battle against the extensive marshlands that surrounded the city and the port suburb of Ostia, they just mistook the source of the diseases that occasionally decimated the population as the fetid air and not the microbe-carrying mosquitoes and other vermin. Like humorism, miasmatic theory wouldn’t be overturned until the advent of germ theory. As late as the 1850s, “bad air” would be blamed for major epidemics in Europe, including a virulent cholera outbreak in London and Paris, as well be a cornerstone of Florence Nightingale’s theories of nursing during the Crimean War.

By the 1st century BC/ 1st century AD, surgical medicine had made significant progress since the medical papyri, and Roman doctors were relatively skilled at a variety of procedures. Physicians were more confident in excising tumors, performing trephinations, and executing most eye-related surgeries. However, anesthetics remained a problem for the ancient Roman surgeon, so his or her speed was valued as much as their dexterity or results.

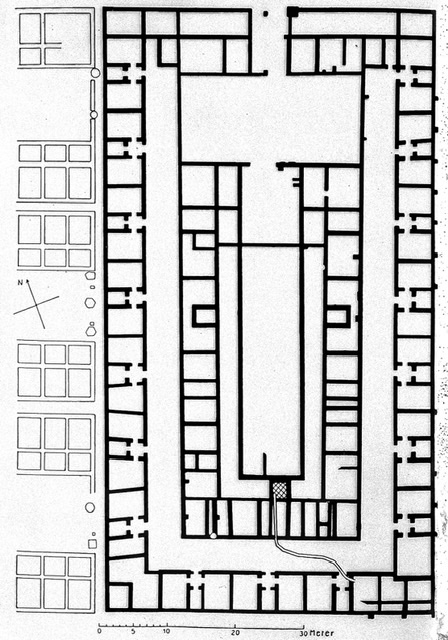
Some of Rome’s greatest contributions to ancient medicine came about because of the empire’s ever-present legions. The Roman army was the first entity to establish something resembling the modern hospital. The valetudinarium was the Roman military field hospital, where physicians would have ample opportunity to observe and treat a vast number of injuries and diseases, knowledge that could in turn be applied under less traumatic circumstances in civilian medicine. On the edges of the Empire, the valetudinarium would become a standard part of Roman fort architecture and their remains show evidence of many features found in a modern hospital such as a triage wing, dispensary, and separate laundry facilities.
But when they weren’t serving in the army, the average Roman preferred to be treated by their doctor at home. This came in part from an ancient tradition that placed medical care in the hands of a family’s paterfamilias, who would employ a combination of native herbs, chants, prayers and charms for healing. Cato’s equally irascible great-grandfather, Cato the Elder, famously lamented the rise of Greek-influenced medical treatment at the expense of Rome’s own medical traditions, probably as just one more way the paterfamilias’ rightful authority was being eroded by nefarious outside forces. Cato Sr. was known to treat his family and dependents personally, most of his remedies apparently involving cabbage in one form or another. Which sounds exactly like something a grumpy old man with limited medical training would prescribe to you.

Leave a comment